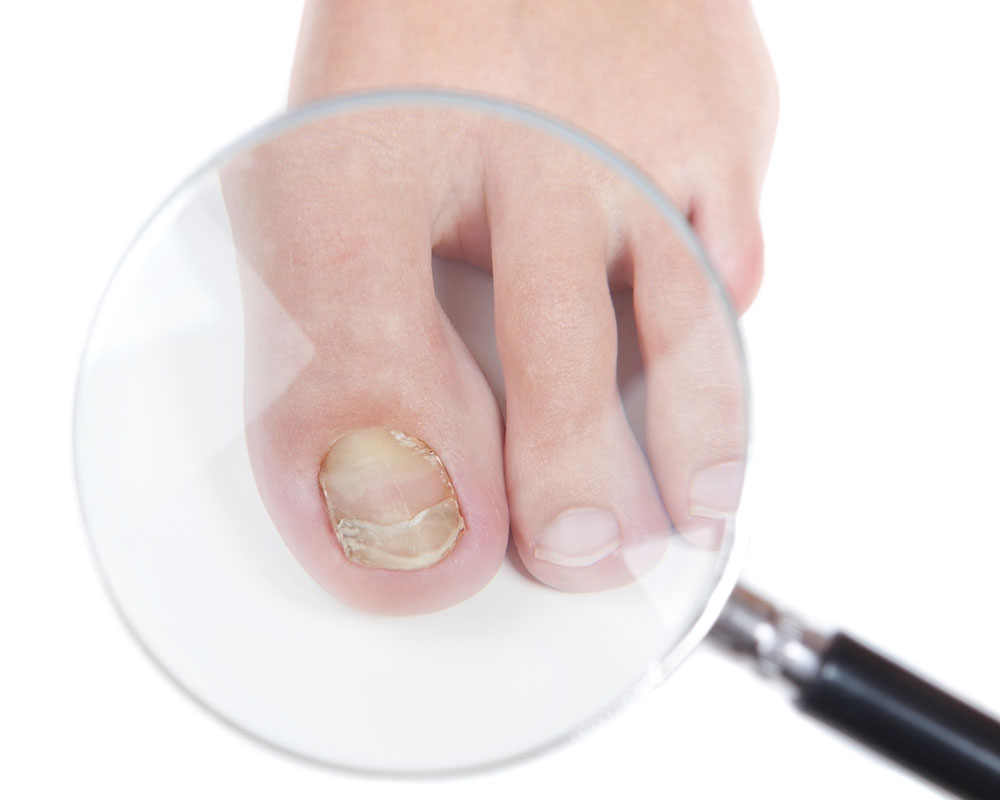
Fungal nail infections
Fungal nail infections are called onychomycosis (from the Greek onychomycosis) and usually represent a chronic fungal infection of the nail plate caused by various types of pathogenic fungi. These fungi feed on keratin, break it down, and may lead to more serious conditions, such as dermatomycosis of the skin.
Prevalence of fungal nail infections
Nail fungus is a fairly common condition. According to international statistics, 10–20% of the world’s population suffer from this disease.
People living in colder climates are more susceptible to onychomycosis. In tropical countries, however, mold fungi are more common. Residents of large cities develop this infection more often than those living in small towns or rural areas. The incidence of the disease also increases with age.
Professions with a higher risk of fungal nail infections include factory workers, miners, power plant employees, military personnel, and athletes. This is largely due to crowded environments, shared locker rooms and showers, and the regular use of uniforms or specialized footwear.
Nail fungus usually does not spread directly from person to person. Instead, it is transmitted indirectly through contaminated surfaces and objects, such as wooden floors in public saunas, communal showers, gyms, personal hygiene items, and similar environments.
Onychomycosis can be caused by around fifty different species of fungi, which are usually divided into three main groups:
- Dermatophytes — This group includes Trichophyton rubrum and Trichophyton interdigitale. Dermatophytes cause about 80% of all fungal nail infections.
- Yeasts — These are fungi belonging to the Candida genus. Yeasts account for 5–10% of active onychomycosis cases and more often affect fingernails.
- Molds. This group includes two major fungal families: Moniliaceae and Dematiaceae. In most cases, these fungi cannot cause nail disease on their own and become pathogenic only in combination with other factors, such as bacterial infections or other pathogens.
Conditions for the development of nail fungus:
Pathogenic fungi can enter the nail plate in different ways. The route of infection and the structures affected determine the visible clinical picture of the disease.
The main types of infection are classified as follows:
- Distal subungual
- Proximal subungual
- Superficial
- Total dystrophic
In distal subungual onychomycosis, the fungus penetrates the nail plate from an infection site on the surrounding skin (often without noticeable symptoms). After entering the nail plate, the fungus spreads to the nail bed, causing thickening and separation of the nail plate (onycholysis). The fungus continues damaging the nail and may eventually reach the nail matrix, leading to a more severe form known as total dystrophic onychomycosis. In most cases, this type of infection is caused by Trichophyton rubrum.
Trichophyton interdigitale, however, penetrates the nail directly through its surface and causes damage known as superficial white onychomycosis. The fungus spreads across the nail plate in the form of irregular white patches and may gradually penetrate through all layers of the nail.
The first and fifth toenails are affected most frequently because they are more exposed to trauma while walking. This type of fungal infection often occurs together with interdigital skin infections between the toes.
The third route of infection occurs through the proximal nail fold. Fungi of the Candida genus most often infect the nail through this pathway. From the nail fold, fungal filaments penetrate the nail matrix and then spread beneath the nail plate, infecting the entire nail bed.
In such cases, the disease often begins acutely, with inflammation affecting the entire nail fold.
Treatment of nail fungus
All treatment methods for nail fungus aim to eliminate the cause of the disease — the pathogenic fungus. Treatments are generally divided into two main groups:
- Topical medications
- Systemic medications
The choice of medication and the treatment plan are determined individually for each patient and must be prescribed by a dermatologist.
There is also a combined treatment approach, which includes both systemic medications (tablets) and local therapy (topical application of antifungal agents directly to the nail).

Prevention of nail fungus
Prevention of onychomycosis is divided into two main categories:
- Public prevention
- Personal prevention
Public Prevention: This involves improving hygiene conditions in public spaces such as swimming pools, saunas, gyms, and other shared facilities. It also includes preventive screening of visitors and risk groups (such as athletes, industrial workers, and military personnel) and public education about hygiene practices.
Personal prevention Personal prevention is divided into primary and secondary prevention.
Primary prevention aims to prevent fungal infection and includes:
- Wearing only personal footwear
- Maintaining consistent foot hygiene
- Using topical antifungal products for individuals who frequently visit public facilities (for example, BAEHR “foot tonic” or “nail and foot protective spray”)
- Early detection and treatment of fungal infections
Secondary prevention applies to individuals who have already had nail fungus. Its goal is to prevent recurrence and includes:
- Careful and consistent foot hygiene
- Preventive use of topical antifungal products for 2–3 months after treatment
- Replacing or disinfecting previously used footwear
- Strengthening the body’s overall immune defense
When treating nail fungus, it is important that the affected part of the nail plate is removed. In this case, medical hardware pedicure and nail reconstruction (prosthetic nail restoration) can be very helpful. In recent years, doctors have increasingly begun to cooperate with podology specialists in the treatment process.
If you have any questions about this topic or would like to purchase products from the world-renowned German brand BAEHR to protect your feet from fungal infections, please contact our clinic.
